 Index
Index

The concentration of blood sugar (glucose) changes throughout the day based on what we eat and our activity level. The normal concentration of blood sugar should be between 70 to 130 milligrams per deciliter (mg/dL) before meals, and less than 180 mg/dL after meals, according to the National Institutes of Health.[1] This corresponds to 3.9 to 7.2 millimoles per liter (mmol/L) before meals and less than 10 mmol/L after meals.
The Fasting Blood Sugar (FBS) is normally tested in the morning after having abstained from food for at least 8 hours. This test is done to check for prediabetes and diabetes. A healthy person will have FBS between 70 and 100 mg/dL because the values can vary depending on physical activity and the method used for testing. Laboratory testing generally uses blood drawn from a vein, whereas home testing uses blood obtained by pricking a finger.
What is glucose?
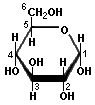
Glucose is a simple carbohydrate that is the brain's principal source of energy.
Our bodies obtain glucose from the carbohydrates in plant products.
Table sugar, for example, is a disaccharide consisting of glucose and fructose.
Starch is a mixture of amylose, a linear polysaccharide,
and amylopectin, a highly branched polysaccharide. Starch is broken down into
glucose by the enzymes in saliva and the small intestine. This is why eating white bread or potatoes,
which are rich in starch, raises the blood sugar very quickly.

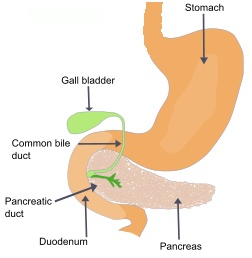
The level of glucose in the bloodstream is regulated by hormones secreted by the islets of Langerhans in the pancreas. The islets contain beta cells that produce insulin, and alpha cells that produce glucagon. When the level of blood sugar increases after a meal, the beta cells release insulin to promote the conversion of glucose to glycogen and fat. Glycogen is a polysaccharide similar to starch which is stored mainly in the liver, but it is also stored in small amounts in the muscles. The glucose that is not stored as glycogen is stored as fat through the process of lipogenesis which converts sugars to acetyl-coenzyme-A as an intermediate toward the formation of fatty acids and triglycerides. The blood sugar level returns to normal once the glucose has been burned or stored as glycogen or fat.
When the blood sugar level drops below normal, the alpha cells in the islets of Langerhans of the pancreas produce glucagon which helps convert stored fat into fatty acids and ketone bodies that can be used by the body for energy. This fat-burning metabolic process is called ketosis. The ketone bodies from fatty acid oxidation can be used by the heart and skeletal muscles for energy, thereby preserving the limited glucose for use by the brain.[2] The release of glucagon is inhibited by the presence of insulin. Frequent snacking or drinking sugary beverages promotes obesity because the body is not given a chance to get into a fat-burning mode.
What is Diabetes?
Diabetes mellitus, commonly called diabetes, is a group of metabolic diseases characterized
by high levels of blood glucose caused by
a deficiency of insulin production or the inability of the body to react to insulin.
Diabetes is very prevalent among overweight and inactive persons and can lead
to serious complications and premature death.
Diabetes symptoms may include unusual thirst, a frequent need to urinate, extreme fatigue
or blurred vision. Approximately 8.3 percent of the
U.S. population has diabetes, but one third of them do not know that they have
the disease.[3]
Prediabetes
Prediabetes is a condition where blood glucose levels are higher than normal but not high enough
to be called diabetes. Persons with "impaired glucose tolerance"
or "impaired fasting glucose" but who have no symptoms of diabetes fall in this category.
Prediabetes is almost always present before the more serious type 2 diabetes develops.
Prediabetes is usually diagnosed with an Oral Glucose Tolerance Test (OGTT). The test is performed by asking the patient to abstain from food for at least 10 hours. An initial blood sample is taken, and the patient is asked to drink a solution with 75 grams of glucose. During the test, the patient needs to lie or sit quietly. Blood samples are taken at 30 minutes, 1 hour, 2 hours, and 3 hours after drinking the high glucose drink. For a normal person, the glucose level will rise and then quickly fall back to normal as insulin is produced in response to the glucose. The blood sugar level of a diabetic person will rise and stay elevated for a long time since insulin is not produced or the cells of the body do not respond to it. The following graph shows typical normal responses to the OGTT over a period of two hours with blood samples taken every 15 minutes during the first hour.

Diabetes Type 1
Type 1 diabetes accounts for approximately 5 percent of all diagnosed cases of diabetes
in adults. Type 1 diabetes was previously called juvenile diabetes or insulin-dependent diabetes.
It is a chronic condition in which the pancreas produces no insulin or does not
produce enough insulin for proper glucose metabolism.
Type 1 diabetes is a progressive autoimmune disease, in which the beta cells that produce insulin
are destroyed by the body's own immune system. It is thought that
genetic predisposition and environmental factors, such as viral infections, may trigger
the mechanism that destroys the beta cells.
Once the islet cells are destroyed, insulin cannot be produced.
Diabetes Type 2
Type 2 diabetes accounts for 90 to 95 percent of all diagnosed cases of diabetes in adults, but
it is increasingly being diagnosed in children and adolescents.
Type 2 diabetes was previously called adult-onset or noninsulin-dependent diabetes.
Type 2 diabetes occurs when the body becomes resistant to the effects of insulin or
does not make enough insulin. Excess weight and inactivity seem to be contributing factors
to the development of this disease.
Type 2 diabetes may develop very slowly. Some common symptoms include increased thirst and
frequent urination, increased hunger, fatigue, blurred vision and slow-healing sores.
There is no cure for type 2 diabetes, but the condition may be managed or even
prevented by exercising and maintaining a healthy weight. When diet and exercise
are not enough to control type 2 diabetes, the blood sugar level has to be managed
with diabetes medications or insulin therapy.
Diet and Exercise
A study of 3,234 overweight participants with prediabetes found that
participants who lost a modest amount of weight through dietary changes
and increased physical activity sharply reduced their chances of developing
diabetes.[4,5] Exercise and diet were more effective than treatment with
metformin (Glucophage) which is a drug taken orally to control diabetes.
The lifestyle intervention group, received intensive training in diet,
physical activity, and behavior modification. By eating less fat and fewer calories
and exercising for a total of 150 minutes a week, they aimed to lose 7 percent
of their body weight and maintain that loss. Another group took 850 mg of metformin
twice a day.
Participants in the lifestyle intervention group, which included men and women from different ethnic groups, reduced their risk of developing diabetes by 58 percent. Participants aged 60 and older who were in the diet and exercise group reduced their risk of developing diabetes by 71 percent. Learn how to lose weight.
Diabetes Medications
In addition to insulin injections, several oral drugs are used to control diabetes.
Oral diabetes pills include sulfonylureas, meglitinides, biguanides,
thiazolidinediones, alpha-glucosidase inhibitors and DPP-4 inhibitors.
The drugs work in different ways to lower blood glucose levels and
sometimes are used in combination.
Sulfonylureas such as glipizide (Glucotrol) and glyburide (Micronase)
stimulate the beta cells of the pancreas to release more insulin.
Meglitinides such as repaglinide (Prandin) and nateglinide (Starlix)
also stimulate the beta cells to release insulin.
Biguanides like metformin (Glucophage)
lower blood glucose levels by decreasing the amount of glucose produced by the liver.
Thiazolidinediones like rosiglitazone (Avandia) improve insulin sensitivity in the
muscle and fat and also reduce glucose production in the liver.
Alpha-glucosidase inhibitors like acarbose (Precose) and meglitol (Glyset)
block the breakdown of starch and sucrose thus slowing down the rise in blood glucose levels.
DPP-4 inhibitors like sitagliptin (Januvia) and saxagliptin (Onglyza)
work by preventing the breakdown
of the naturally occurring compound glucagon-like peptide-1 (GLP-1) which
reduces glucose levels.
Oral diabetes pills are typically taken before meals.
Complications from Diabetes Medicines
In 2010 the FDA placed the diabetes medicine Avandia under severe restrictions, stating that it should be only
used as a last resort in treating people with diabetes. Avandia was found to raise the risk of heart attack by
40 percent in people taking the drug.
The FDA has been looking into claims that there is an association between the diabetes medicine
Januvia and pancreatic cancer and research is being done to further back the claim.
Januvia has been linked to increased
attacks of pancreatitis in users.[6] Chronic pancreatitis can lead to the development of pancreatic cancer.
The diabetes drug Actos has been shown to reduce bone density in the hips and spine of women taking the drug,
as well as raising the risk of developing eye problems like macular edema.
The safest forms of diabetes medication have proven to be Glucophage (metformin) and Glucotrol (glipizide). Any peculiarities you may have been experiencing should be discussed with your doctor, who may change your medication to try and alleviate any difficulties you may be having.